Tongue Ties
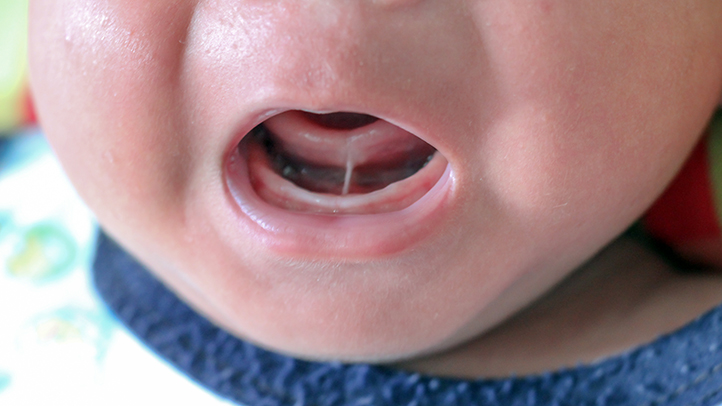

Tongue tie — known medically as ankyloglossia — is a condition present from birth in which a small band of tissue called the lingual frenulum is shorter, tighter, or positioned further forward than usual. This restricts the tongue’s movement and can significantly interfere with a baby’s ability to feed effectively.
To feed well, a baby needs to extend their tongue over their lower gum, create a wide, deep latch, and use a rhythmic wave-like movement to draw milk. This is hard, coordinated work — and the tongue is at the centre of all of it. When tongue movement is restricted, that whole process breaks down. The baby compensates by clamping, chewing, or gripping with their lips, which leads to pain for the feeding parent, inefficient milk transfer for the baby, and frustration for both of you.
This is one of the most important things to understand — and one of the main reasons tongue tie is so frequently missed.
Anterior tongue ties are the most visible. The frenulum runs close to or right to the tip of the tongue, which may look heart-shaped or notched when lifted. These are more likely to be picked up at routine newborn checks.
Posterior tongue ties are far more subtle. The frenulum sits further back under the mucous membrane at the base of the tongue, making it invisible to a simple visual check. The tongue may appear entirely normal at first glance. Yet posterior ties can cause every bit as much feeding difficulty as anterior ones — sometimes more — and are routinely missed by healthcare professionals who haven’t been specifically trained to find them.
This is why a proper, functional assessment — not just a quick look in the mouth — is so important.
No two babies present in exactly the same way, and not every baby with a tongue tie will show every sign on this list. But if several of these resonate with your experience, a tongue tie assessment is absolutely worth pursuing.
Tongue tie is not just a baby problem. It is a feeding problem, and that means your experience matters just as much. Please don’t dismiss your own symptoms.
That last one matters. You know your baby. If your instinct says something isn’t right, trust it and seek an assessment.
A proper tongue tie assessment is nothing like a quick glance in the mouth. It is a thorough, clinical process that takes the whole feeding picture into account — and this is where my background as both an IBCLC and an experienced neonatal nurse makes a real difference.
Your assessment with me includes:
A detailed feeding history. Before I look at anything, I listen. I want to understand your full feeding experience — when difficulties started, what they feel like, what you’ve already tried, and how both you and your baby are coping. This context shapes everything that follows.
Observation of a complete feed. I watch your baby feed in real time — at the breast or bottle — assessing latch, positioning, tongue movement, lip seal, swallowing pattern, and behaviour throughout the feed. This is often where the most important information comes from.
Full oral assessment. I carry out a hands-on examination of your baby’s mouth, assessing the structure and — crucially — the function of the tongue. I assess how the tongue lifts, extends, and moves, not simply how it looks. This is how posterior ties, in particular, are identified.
Clear explanation of findings. I will explain exactly what I’ve found in straightforward language, what it means for your baby’s feeding, and what I would recommend. If a tongue tie is present and affecting feeding, I will discuss division as an option. If I don’t believe intervention is warranted, I will tell you that honestly too — and I’ll explain why.
A written report. You’ll receive a written summary of my assessment findings and recommendations to keep for your own records and share with your GP, health visitor, or midwife if needed.
If assessment confirms that a tongue tie is present and is contributing to feeding difficulties, I can carry out the division — a simple procedure called a frenulotomy — as part of the same appointment or at a follow-up visit.
In young babies, typically under six months, frenulotomy is a quick, safe, and well-tolerated procedure. Using sterile scissors, I divide the frenulum under the tongue. The tissue in young infants is thin, has very few nerve endings, and heals rapidly. The procedure takes only a matter of seconds.
A small amount of bleeding is entirely normal and resolves quickly. Most babies cry briefly — often more from the handling than the procedure itself — and the majority settle quickly, ideally at the breast, immediately afterwards.
I know this sounds daunting. Almost every parent I see feels anxious beforehand. And almost every parent tells me afterwards that it was far less distressing than they had feared.
Feeding support immediately after the procedure is just as important as the division itself. Because I am both a tongue tie practitioner and an IBCLC, I don’t hand you a leaflet and send you on your way. I stay with you, support the first feed post-division, and help you and your baby begin to find a new feeding rhythm with greater tongue freedom.
Some babies show an improvement immediately. For others, it takes a few days or even a couple of weeks as they learn to use their tongue in a new way — unlearning the compensatory habits they’ve developed. I’ll be honest with you about what to expect and when.
After division, I’ll provide guidance on wound management exercises — gentle stretches that help prevent the tissue from reattaching as it heals. These take only moments and are an important part of getting the best possible outcome.
I also offer follow-up support in the days and weeks after the procedure. Feeding after tongue tie division can take time to settle fully, and having ongoing access to IBCLC-level support during that period can make a significant difference to your long-term feeding outcomes.
One of the biggest frustrations parents face when navigating tongue tie is being referred between multiple different practitioners — a GP who isn’t sure, a health visitor who can’t assess, a tongue tie service with a long waiting list, a separate lactation consultant for the feeding support.
Because I hold both my IBCLC qualification and my tongue tie practitioner qualification, I offer something genuinely different: one specialist, one relationship, the complete picture.
I assess. I advise. I divide when it’s indicated. And I support your feeding before, during, and after — with the clinical background of someone who has spent thirteen years caring for newborns at the most complex end of neonatal care.
You don’t need to start from scratch with someone new at each step. You don’t need to re-explain your history. You don’t need to wait weeks between an assessment and a follow-up appointment. I’m with you through the whole journey.
No — and I think it’s important to say that clearly.
Division is recommended only when a tongue tie is identified and is causing clinically significant feeding difficulties. The presence of a tie alone is not sufficient reason to divide. Some babies have ties that cause no problems whatsoever and require no intervention.
My role is always to give you an honest, evidence-based picture of what I find and what I genuinely recommend — not to over-treat, and not to dismiss. Every family I work with deserves a thoughtful, individualised assessment, and that is exactly what I provide.
I see babies from birth up to 12 weeks for tongue tie division, and I’m happy to carry out assessments and provide feeding support for older babies and children too.
I work with:
If you’re not sure whether a tongue tie assessment is right for your situation, please don’t hesitate to get in touch. A quick conversation is often all it takes to work out the best next step.
You don’t have to keep struggling, and you don’t have to wait and hope things improve on their own. Early assessment and support can make an enormous difference — to your feeding experience, to your baby’s comfort, and to your confidence as a parent.
I offer home visits across East Sussex and Zoom consultations for initial feeding assessments. Tongue tie assessments and divisions are carried out as home visits.