You’ve just brought your baby home. You’re exhausted, emotional, and doing your absolute best. But breastfeeding — something you were told would be “natural” — feels anything but. Your nipples are sore, your baby seems frustrated at the breast, and every feed leaves you both in tears. You find yourself wondering: is something wrong with us?
The answer, in many cases, is that nothing is wrong with either of you. But there may be a small physical reason why feeding is such a struggle — and it’s called a tongue tie.
Tongue tie is one of the most common yet frequently missed causes of breastfeeding difficulties in newborns. As a lactation consultant working with families across East Sussex, I see it regularly — and the relief parents feel when they finally have an explanation is palpable. So let’s talk about what tongue tie actually is, how to spot it, and what your options are.
What Is a Tongue Tie?
Tongue tie, or ankyloglossia to use its medical name, is a condition that’s present from birth. Normally, the tongue is attached to the floor of the mouth by a small piece of tissue called the lingual frenulum. In most people, this frenulum is thin, flexible, and positioned far enough back that it doesn’t interfere with how the tongue moves.
In babies with tongue tie, however, this frenulum is shorter, tighter, or positioned further forward than usual. This restricts the tongue’s movement — and when you consider just how hard a baby’s tongue has to work during feeding, you begin to understand why this can cause real problems.
A baby feeds effectively by extending their tongue over the lower gum, cupping the breast, and using a wave-like motion to draw milk. If the tongue can’t move freely, that whole process is disrupted. The baby may clamp down with their gums instead, slip off the breast repeatedly, or exhaust themselves trying to get enough milk.
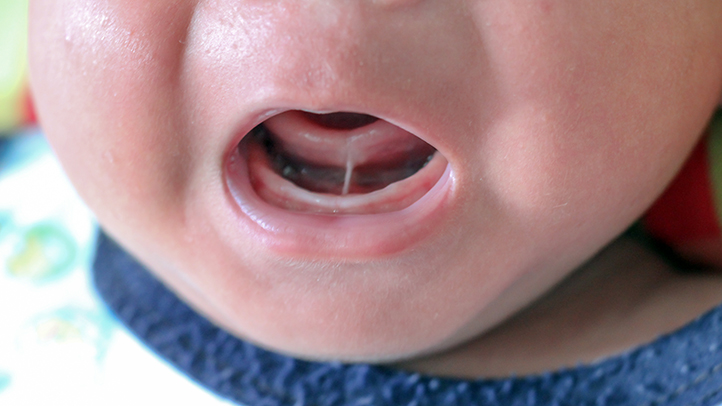
It’s worth knowing that tongue ties exist on a spectrum. Some are immediately obvious — a classic “anterior” tongue tie where the frenulum runs right to the tip of the tongue, sometimes giving it a heart-shaped appearance when lifted. Others are far more subtle — what’s known as a “posterior” tongue tie, tucked beneath the mucous membrane at the base of the tongue and easily missed by an untrained eye. These posterior ties are particularly commonly overlooked, yet they can cause just as much difficulty.
How Common Is It?
Tongue tie affects somewhere between 4% and 11% of newborns, depending on which studies you read — and it’s thought to run in families. Boys are more commonly affected than girls. It is, in other words, not rare. Yet it is not routinely checked for at newborn checks, as examiners are not trained to accurately diagnose a tongue tie. This can leave families to struggle without answers, sometimes for weeks.
Signs That Your Baby Might Have a Tongue Tie
Every baby is different, and not every baby with a tongue tie will experience every symptom on this list. But here are the signs I’d encourage you to take seriously.
Signs in your baby:
- Difficulty latching on, or latching and then sliding off the breast repeatedly
- A clicking or clucking sound during feeding
- Seeming constantly hungry, even after long feeds
- Taking a very long time to feed — often over 40 minutes
- Excessive wind, reflux-like symptoms, or a very gassy tummy (caused by swallowing air during inefficient feeding)
- Poor weight gain or slow return to birth weight
- Frustration and crying at the breast
Signs in you:
This is important, because tongue tie is not just a baby problem — it’s a feeding problem, and that means it affects you too.
- Nipple pain during or after feeds (nipples that come away looking flattened, lipstick-shaped, or blanched)
- Cracked or bleeding nipples that aren’t improving
- Recurring blocked ducts or mastitis
- A feeling that your baby is “chewing” rather than suckling properly
- Low milk supply developing over time — often a consequence of inefficient milk removal
- Dreading feeds, or feeling like you’re failing, when actually the mechanics simply aren’t working
If several of these resonate with you, please don’t dismiss them. These are real, valid symptoms — and they deserve proper assessment.
How Is Tongue Tie Diagnosed?
This is where things can get frustrating for parents. In the UK, tongue tie should ideally be assessed by a trained practitioner — a tongue tie practitioner, lactation consultant, or specialist midwife who has been specifically trained to carry out a full oral assessment.
A proper assessment isn’t just a quick look in the mouth. It involves watching a feed, assessing the baby’s latch, checking the function of the tongue (not just its appearance), and considering the whole picture of feeding. This is why a visual check alone — the kind that might happen at a postnatal ward check — often isn’t enough to identify subtler ties.
If you have concerns, you can ask your midwife or health visitor for a referral, contact your local tongue tie service directly, or reach out to a lactation consultant who can carry out an assessment and refer on if needed. You don’t have to wait and hope things improve on their own.
What Are the Treatment Options?
If a tongue tie is identified and is causing feeding difficulties, the most common treatment is a simple procedure called a frenulotomy (also called a frenotomy or division).
In young babies — typically under 6 months — this is usually a very quick and straightforward procedure. The frenulum is snipped with sterile scissors or a laser by a trained practitioner. In newborns, the tissue is thin and has very few nerve endings, so the procedure takes only a few seconds, involves minimal bleeding, and most babies settle quickly at the breast afterwards.
It sounds scary. I completely understand why. But many parents describe it as far less dramatic than they feared, and the improvement in feeding can be remarkable — sometimes noticed within the first feed after the procedure, though more commonly over the following days and weeks as your baby learns to use their tongue in a new way.
It’s also worth knowing that division isn’t always the automatic answer. If a tongue tie is identified but feeding is going well, intervention may not be necessary. The goal is always to support feeding — so the decision should be made based on the full clinical picture, your baby’s symptoms, and your own feelings, never on the presence of a tie alone.
After a division, feeding support is really important. Tongue exercises (sometimes called “wound management exercises” or stretches) are usually recommended to prevent the tissue reattaching. And working with a lactation consultant in the days and weeks following the procedure can make a huge difference in helping you and your baby re-establish comfortable, effective feeding.
What If My Baby Isn’t Breastfed?
Tongue tie can also affect bottle-fed babies — causing similar symptoms like excessive wind, slow feeding, and difficulty maintaining a seal on the teat. It can also go on to affect speech development, eating, and even oral health as a child grows, though the evidence on long-term impacts is still evolving. If you have concerns about your formula-fed baby, they are just as valid and just as worth exploring.
You Are Not Failing
I want to pause here and say something clearly: if you are struggling with breastfeeding and wondering whether tongue tie might be involved, you are not failing. You are not doing it wrong. You are not weak for finding it hard.
Breastfeeding is a skill — for both of you — and when there’s a physical barrier in the way, no amount of determination alone will fix it. Seeking help is the most proactive, loving thing you can do for yourself and your baby.
When to Seek Support
If any part of this post has spoken to your experience, please don’t wait for things to improve on their own. Early support really does make a difference.
Reach out to:
- Your midwife or health visitor for an initial check and potential referral
- An IBCLC lactation consultant for a full feeding assessment (I offer home visits across East Sussex and Zoom consultations if you’re further afield)
- Your local tongue tie service — many can be accessed directly without a GP referral
You deserve feeding support that actually helps. And your baby deserves a comfortable, nourishing start to life. With the right help, that is absolutely possible — even if right now it doesn’t feel that way.
Louise Bicknell is an IBCLC-certified lactation consultant based in Polegate, East Sussex, offering home visits and online consultations. If you’d like to book an assessment or simply have a chat about your feeding concerns, get in touch — she’d love to help.